The Navigator’s Circle

A New Kind of Leadership Community Is Here The Problem Nobody’s Talking About You’re drowning in tools. Your inbox is a graveyard of half-integrated platforms. Your team is fragmented across a dozen different systems. And the worst part? You’re paying for all of it while your actual leadership challenges go unsolved. The Navigator’s Circle isn’t another software platform. It’s a curated community of forward-thinking leaders who’ve decided that success isn’t about having more tools—it’s about having the right people in the room. What Members Are Actually Experiencing Result Timeline Typical Impact 3X productivity increase First 60 days Teams operating with unprecedented efficiency 25% reduction in leadership overhead First quarter C-suite reclaims strategic focus 3 new high-performing hires First 6 months Network-sourced talent, zero recruiter fees $200K+ in avoided expenses Year one Fractional expertise replaces full-time hires For C-Suite Executives: Strategic Advantage You need clarity on what’s working and what’s wasting money. The Navigator’s Circle gives you direct access to fractional C-level advisors, battle-tested frameworks, and a peer group who’ve solved your exact problems. No consultants. No fluff. Just operators who’ve been where you are. What you get: The outcome: Decisions that move faster. Leadership that scales. Growth that doesn’t require hiring more managers. For Operations Managers: Implementation Wins You’re responsible for making strategy actually happen. That’s where most leaders fail. The Navigator’s Circle connects you with implementation specialists who’ve automated away the busywork, recruited impossible hires, and built systems that let small teams punch above their weight. What you get: The outcome: Your team does 3X the work without hiring 3X the people. You become the operations leader everyone wants to work for. For Visionary Founders: Acceleration Blueprint Building something new requires navigating chaos that textbooks don’t prepare you for. The Navigator’s Circle is your shortcut to wisdom from founders who’ve navigated what you’re facing now. Real product-market fit insights. Real scaling strategies. Real capital conversations. What you get: The outcome: You skip the two-year learning curve. You raise capital faster. You build something that lasts. Real Leaders. Real Results. Real Impact. Sarah Chen, VP of Operations: TechScale Ventures “We implemented the Navigator’s Circle framework in Q2. By Q4, our team was operating at 6X the productivity with half the management overhead. That’s not hyperbole—that’s our actual metrics. Sarah Chan, VP of Operations, TechScale Ventures” Marcus Williams, CEO: Growth Capital Partners “The peer advisory board alone justified membership. I’ve made three strategic decisions this year that directly trace back to conversations in the Circle. One of them saved us $800K on a failed market expansion.” Jennifer Park, Founder & CEO: Park Innovation Labs “As a first-time founder, I thought I needed a fancy advisory board. Turns out I needed the Navigator’s Circle. The recruiting playbooks alone have brought in a team I couldn’t have built in 24 months anywhere else. And I paid a fraction of what a traditional board would cost.” David Ortiz, Chief Operations Officer: Summit Technologies “The automation templates were plug-and-play. Our operations team deployed them in three weeks. The real value? Having a peer group who gets what you’re actually dealing with—not a consultant who bills by the hour.” Elena Rodriguez, Chief Strategy Officer: Velocity Ventures “I’ve been part of exclusive networks before. This is different. The Navigator’s Circle is built for operators who want to move fast and make decisions that matter. The strategic frameworks are battle-tested. The people are real.” Here’s What Makes This Different ** Not another mastermind group** — We’re past the era of standing around sharing war stories. The Navigator’s Circle is built on documented systems, tested frameworks, and real accountability. ** Not a software subscription** — We integrate the tools you need (CRM, automation, video engagement, virtual assistance, recruiting systems, fractional leadership). The Circle is the people ecosystem that makes those tools actually work. ** Not for everyone** — We’re selective. Your peers matter more than your membership fee. We maintain a strict ratio of operators-to-services to ensure quality and cohesion. ** Built for rapid growth** — Members see measurable impact in 30 days, not 30 months. ** Powered by real frameworks** — 50+ proven playbooks covering everything from CRM optimization to fractional team scaling. ** Your peer board** — Direct access to fractional C-level advisors, founder networks, and operational specialists. Limited Founding Member Spots Available We’re launching The Navigator’s Circle with just 50 founding member positions. This is intentional. Once we hit 50, the doors close until Q3 2026. Why limited? Scaling a peer community too fast kills the magic. You end up with a conference, not a circle. We’re committing to keep this tight, curated, and high-velocity. Founding members lock in: 12 founding member spots remain. The Ask Is Simple You get 30 days to experience the full Circle. No risk. No commitment beyond that month. You’ll have: If it’s not worth 10X the membership fee by day 30, you get your money back. We’re not worried about that offer because every member we’ve beta-tested with has gone deeper. Start Here: Join the Founding Circle [Join as a Founding Member — Limited Spots] No long-term contracts. 30-day trial. Money-back guarantee. Your peer group is waiting. The frameworks are ready. The only question is: Are you ready to move faster than your competition? Questions? Let’s Talk. [Schedule a 15-Minute Conversation] We’ll walk you through what membership looks like, answer any questions, and help you decide if the Navigator’s Circle is the right move for your organization right now. No pitch. No pressure. Just a real conversation about what you’re trying to build. The Navigator’s Circle: Where strategy meets execution. Where peer wisdom meets proven frameworks. Where growth happens faster than you thought possible. [Join the 50 → Only 12 Spots Remain] Why Now? The world has fundamentally changed. Traditional advisory boards are slow, expensive, and often disconnected from how companies actually operate today. Mastermind groups are ineffective without framework discipline. Most peer networks are just expensive happy hours. The Navigator’s Circle is built for the way leaders actually work in 2026: This is leadership for the next generation of builders. Last updated: February 9, 2026 | The Navigator’s Circle |
Master Your Time, Master Leadership: Eisenhower Matrix for Executives
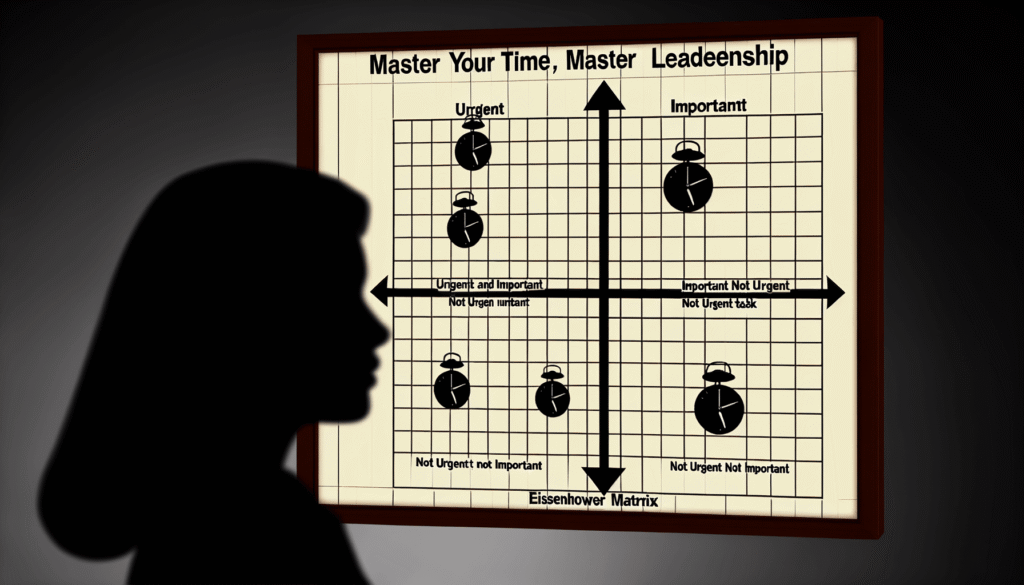
Why the most effective leaders aren’t busier, they’re strategically focused on what actually matters The Executive Paradox: Why Being Busy Isn’t the Same as Being Effective You’re drowning in tasks. Your calendar is packed from 7 AM to 7 PM. Your inbox never reaches zero. And yet, at the end of each week, you struggle to point to the strategic progress that actually moves your organization forward. You’re not alone. Research shows that executives spend roughly 41% of their time on activities that could be handled by someone else or eliminated entirely. That’s nearly two full days every week spent on low-impact work while your most important strategic initiatives languish in your “someday” folder. The culprit? What psychologists and productivity researchers call the urgency trap: the seductive belief that because something is urgent, it must be important. Your phone rings. Your inbox pings. A crisis emerges. And suddenly, your carefully planned strategy for the quarter gets shelved while you firefight another emergency. President Dwight D. Eisenhower faced this exact problem. As Supreme Allied Commander and later as President, he had to manage competing demands from dozens of stakeholders, each convinced their request was the most critical priority. In 1954, he articulated a deceptively simple principle that would become the foundation for one of the most powerful leadership frameworks ever created: “What is important is seldom urgent, and what is urgent is seldom important.” That distinction, and the matrix that emerged from it, separates exceptional leaders from perpetually overwhelmed ones. This is what the Eisenhower Matrix teaches us. And if you implement it correctly, it will fundamentally reshape how you lead, how you work, and ultimately, how much impact you have on your organization. Understanding the Eisenhower Matrix: Your Leadership Operating System The Eisenhower Matrix is deceptively simple in design but profound in application. It’s a 2×2 framework that categorizes every task, project, and decision you face into one of four quadrants based on two variables: urgency (does this need immediate attention?) and importance (does this directly impact my strategic objectives?). Let’s break down each quadrant and what it means for your leadership: Quadrant 1: Urgent & Important: Crisis Management (DO FIRST) These are your genuine emergencies. The client who’s threatening to walk. The system that’s gone down. The compliance issue that just surfaced. The competitive threat that appeared overnight. Characteristics: Executive Examples: The Reality: Q1 work is inevitable. Every leader faces genuine crises. The problem isn’t that Q1 exists, it’s that many executives spend 60-80% of their time here when it should typically be 15-20% of your focused effort. Q1 attracts your attention because it’s visceral. It triggers stress hormones. It feels productive to address it. But here’s the critical insight: the size of your Q1 quadrant is largely determined by how much time you invest in Q2. Quadrant 2: Important & Not Urgent: Strategic Leadership (SCHEDULE—This Is Where Leaders Lead) This is where the magic happens. This is where you’re not reacting to circumstances—you’re creating them. Q2 includes the work that shapes your organization’s future, prevents crises before they emerge, and defines your legacy as a leader. It’s the strategic planning that prevents market disruption. It’s the relationship building that prevents key talent from leaving. It’s the systems improvement that prevents the next crisis. Characteristics: Executive Examples: Why This Matters Most: Satya Nadella transformed Microsoft from a company in decline to a cloud computing powerhouse by investing massive Q2 effort into cloud strategy when it wasn’t yet urgent. The market wasn’t demanding it yet. Wall Street wasn’t asking for it yet. But Nadella understood that this work—this prevention, this strategic positioning—would determine Microsoft’s future. Today, Microsoft’s cloud business generates over $80 billion in annual revenue. That’s Q2 work. That’s leadership. Here’s the uncomfortable truth that most executives resist: if you’re not spending at least 25-30% of your strategic time in Q2, you’re not leading—you’re managing crises. And you’re creating the conditions for more crises tomorrow. Quadrant 3: Urgent & Not Important: Delegation Gold Mine (DELEGATE) These are the tasks that scream for attention but don’t actually require your executive judgment. The meeting that must happen today but doesn’t need you in the room. The report that’s due tomorrow but someone else can write it. The email that needs a response but doesn’t need your personal involvement. Characteristics: Executive Examples: The Delegation Opportunity: This is where the 70% delegation rule transforms your leadership capacity. Here’s how it works: if someone on your team can do the task 70% as well as you would, delegate it. Not when they can do it 90% as well. Not when they can do it perfectly. When they can do it 70% as well. Why 70%? Because the 30% gap is vastly outweighed by the benefit of you having time for Q2 work. A slightly imperfect Q3 task is worth 10 hours of your time freed up for strategic work. Do the math on your hourly value as an executive, that trade is always in your favor. This is how executives who “have no time” suddenly find 10-15 hours per week for strategic work. It’s not magic. It’s delegation discipline. Quadrant 4: Neither Urgent Nor Important: Elimination (DELETE) These are the time wasters. The meetings that have no clear purpose. The reports no one actually reads. The tasks you do out of habit rather than necessity. The activities that feel productive but produce zero value. Characteristics: Executive Examples: The Elimination Principle: Every item in Q4 is an opportunity to reclaim time. Senior executives who master the Eisenhower Matrix become ruthless about elimination. “Does this directly support our strategic objectives?” If the answer is no, it gets deleted. It’s that simple. Why the Eisenhower Matrix Matters Right Now Eisenhower developed this framework 70 years ago, but its relevance has only intensified in the modern executive environment. The Acceleration Problem Your world moves faster than ever. The time between when a competitive threat emerges and when it impacts your business has compressed from months to weeks. The pace of organizational change has accelerated. Technology disruption feels constant. In this environment, waiting for crises to determine your
The Medical Startup Survival Guide: Why You Need Business Navigators from D+1

How peer collaboration transforms the brutal 3-7 year journey from brilliant idea to market success. Medical startups face unique challenges in strategy execution, regulatory readiness, and scalable growth, and that’s where Business Navigators Consulting helps founders move from ideation to execution. The $2.8 Trillion Problem Your revolutionary medical device could save thousands of lives. Your healthcare AI could transform patient outcomes. Your biotech breakthrough could redefine treatment protocols. But here’s the harsh reality: 73% of digital transformation initiatives fail, and medical startups face even steeper odds. The medical industry startup journey is uniquely brutal. While tech startups can pivot quickly and fail fast, medical entrepreneurs face a 3-7 year minimum timeline just to reach market entry. One regulatory misstep, one failed validation study, or one botched hospital integration can cost millions and years of progress. The question isn’t whether you’ll face impossible challenges. The question is: will you face them alone? The Five-Stage Gauntlet Every Medical Startup Must Navigate Medical startups follow a predictable but treacherous path through five distinct stages: Stage 1: Pre-Seed (Concept and Research) Stage 2: Seed (Product Development and Validation) Stage 3: Early Growth (Clinical Validation) Stage 4: Market Entry (Regulatory Approval and Launch) Stage 5: Scaling (Adoption and Integration) The brutal math: Each stage compounds the previous challenges, creating a survival rate of less than 10% from ideation to successful scaling. Why Traditional Business Support Fails Medical Startups Most business accelerators and consulting firms treat medical startups like typical tech companies. They focus on: The result? Medical startups get advice that sounds logical but proves disastrous in healthcare’s unique ecosystem. Medical entrepreneurs face three specific challenges that generic business support can’t address: How Business Navigators Transforms Medical Startup Success Business Navigators operates on a fundamentally different model: peer-to-peer collaboration rather than traditional consulting. For medical startups, this approach is game-changing. The Peer Advantage in Medical Innovation Why it works: Medical startup founders face challenges that only other medical entrepreneurs truly understand. A SaaS founder can’t advise on FDA pre-submission meetings. A fintech CEO doesn’t grasp hospital procurement cycles. But a peer who’s navigated regulatory approval? Invaluable. Collaborative Problem-Solving for Complex Challenges Business Navigators’ membership-based peer groups provide: The Community Multiplier Effect Unlike traditional consulting where you pay for one expert’s opinion, Business Navigators gives you access to an ecosystem of experience: Real-World Impact: Where Business Navigators Makes the Difference Stage 1-2: Foundation and Development Traditional approach: Hire expensive consultants for regulatory strategy Business Navigators approach: Connect with peers who’ve been through FDA pre-submission process, sharing actual submission templates and lessons learned Result: Save 6-12 months and $100K+ in regulatory consulting fees Stage 3: Clinical Validation Traditional approach: Go it alone with CRO recommendations from online research Business Navigators approach: Tap peer network for CRO referrals, study design reviews, and endpoint selection guidance Result: Avoid $500K+ study redesigns and timeline delays Stage 4-5: Market Entry and Scaling Traditional approach: Standard sales and marketing playbook Business Navigators approach: Learn from peers who’ve successfully navigated hospital procurement, built relationships with key opinion leaders, and achieved payor coverage Result: Accelerate adoption timeline by 12-18 months and avoid millions in wasted market entry spend The Strategic Investment That Pays for Itself For medical startup executives, Business Navigators isn’t just another business service. It’s strategic risk mitigation with measurable ROI: Consider this: If Business Navigators helps you avoid just one major regulatory setback or accelerates market entry by six months, the membership investment delivers 10x+ returns. Conclusion: Don’t Navigate the Medical Startup Journey Alone The path from medical innovation to market success is littered with brilliant ideas that never reached patients. The difference between success and failure often comes down to one factor: having the right guidance at critical moments. Business Navigators’ peer-driven ecosystem gives medical startup founders what they need most: access to people who’ve walked this exact path and survived to share their wisdom. Your breakthrough medical innovation deserves every advantage. In an industry where one mistake can cost years and millions, can you afford to navigate without the collective wisdom of peers who’ve already succeeded? Ready to transform your medical startup journey? Join the Business Navigators community and connect with the peers who can help you avoid the pitfalls and accelerate your path to market success. Because in medical innovation, collaboration isn’t just helpful, it’s essential for survival. Ready to Scale Your Medical Startup with Confidence? Join the Navigator’s Circle and gain the strategy, systems, and expert ecosystem built to move medical innovators from ideation to execution. Book Your Discovery Session
Scaling into Chaos: The Hidden Cost of Healthcare Growth

Healthcare growth doesn’t fail from lack of effort. It fails from lack of governance. Without clear decision rights, risk controls, and accountability structures, expansion creates chaos, compliance exposure, and operational breakdown instead of strength. overnance. The Silent Killer of Healthcare Growth Your organization isn’t failing because your team lacks dedication. Healthcare professionals work harder than almost any industry. You’re not failing because you lack vision or market opportunity. The problem is more insidious: you’re scaling without governance architecture. Every new system, vendor, staff member, and process adds complexity. Without structural clarity, that complexity compounds into a web of confusion. Teams make decisions in silos. Authority becomes unclear. Risk multiplies silently. What started as controlled expansion drifts into reactive firefighting. The difference between healthcare organizations that scale successfully and those that stumble isn’t effort or resources. It’s intentional governance design. Beyond Good Intentions: Engineering Control Into Growth Business Navigators doesn’t retrofit governance after problems emerge. We engineer it into the foundation of expansion from day one. This isn’t about slowing down growth with bureaucracy. It’s about creating the structural clarity that allows you to grow faster and safer. The framework consists of eight interconnected components that transform chaotic scaling into controlled, predictable expansion. Crystal Clear Authority: Decision Rights and Accountability Decision Rights MatricesIn high-growth healthcare environments, ambiguity around decision authority becomes a silent risk multiplier. When teams move quickly but nobody knows who ultimately decides, delays and conflicts emerge. In regulated industries like healthcare, this confusion escalates into compliance exposure. Formal decision rights matrices define with precision: Who has authority over vendor selectionWho approves technology integrationsWho controls budget allocationWho determines patient communication standardsWho owns compliance signoffWho has final authority on timeline shifts This eliminates informal power structures and prevents “shadow decision-making” where authority flows through relationships rather than defined roles. Speed doesn’t override accountability – it’s enabled by it. RACI Accountability Structures Beyond authority, execution requires ownership. RACI (Responsible, Accountable, Consulted, Informed) models assign: A single accountable owner for each initiativeClearly defined responsible parties for executionRequired consultation stakeholdersInformational awareness participants In healthcare growth, initiatives like CRM deployment, HIPAA messaging integration, or clinic onboarding span marketing, operations, compliance, and finance simultaneously. Without RACI structure, duplication, missed tasks, and miscommunication proliferate. RACI alignment ensures execution becomes structured rather than personality-driven. Proactive Risk Management: Visibility Before Crisis Living Risk Registers Healthcare organizations operate where risk isn’t theoretical – it’s measurable and enforceable. Instead of reacting to incidents, leadership needs visibility into potential failure points before they escalate. Living risk registers categorize exposure across six critical areas: Risk Category Focus Area Key Metrics Compliance HIPAA, state regulations Violation probability, penalty exposure Operational Process failures, capacity limits Impact on patient care, revenue loss Financial Budget overruns, revenue gaps Dollar impact, timeline effects Vendor Third-party dependencies Contract risks, SLA failures Reputational Public perception, patient trust Media exposure, patient complaints Data Security Breach risks, access control PHI exposure, system vulnerabilities Each risk entry includes description, probability, impact, owner, mitigation strategy, and review cadence. This transforms risk management from reactive crisis response to proactive operational oversight. Vendor Governance TrackingAs healthcare organizations grow, vendor relationships multiply exponentially. CRM providers, messaging platforms, telehealth systems, billing vendors, cloud services, automation tools – each introduces contractual and compliance exposure. Structured vendor governance tracking documents: Active vendor contracts and renewal timelinesBusiness Associate Agreements (BAAs) for HIPAA complianceAccess permissions and data-sharing boundariesSLA performance metrics and breach protocolsThis ensures no vendor operates outside documented oversight, especially critical in HIPAA regulated environments where third-party processors represent shared liability. Data Protection: Engineering Privacy Into Operations PHI Boundary MappingProtected Health Information cannot drift through unregulated systems. Rather than hoping for compliance, we map PHI boundaries intentionally: Which systems are authorized to store PHIWhich systems may transmit PHI securelyWhich systems must only handle de-identified dataWhere notifications must reference secure portals instead of including dataWhich automations are permitted to interact with sensitive fieldsThis creates a visual and procedural firewall between clinical systems and operational systems. Compliance isn’t assumed – it’s diagrammed and enforced. System of Record Ownership One of the most common drivers of organizational fragmentation is unclear system-of-record ownership. When multiple platforms store overlapping data, version conflicts arise. Reporting becomes inconsistent. Leadership loses confidence in metrics. Formal system-of-record designation covers: Patient data (EHR as authoritative source)Financial data (accounting system primacy)HR records (HRIS system control)Marketing performance (CRM metrics authority)Operational workflows (process management tools)Each category has one authoritative source. Other systems may sync metadata but don’t replace the system-of-record. This preserves data integrity and eliminates reporting discrepancies. Operational Excellence: Controlled Automation and Clear Escalation Automation Approval Frameworks Automation accelerates operations – but unmanaged automation accelerates risk. Structured automation governance requires: Documentation of automation logic and triggering conditionsClear identification of data sources and destinationsVerification that no PHI crosses into unauthorized systemsApproval prior to activation with defined review cyclesPeriodic review of active automations for continued relevanceThis prevents “automation sprawl” where integrations are built informally and later forgotten. Every automation has a purpose, an owner, and a review cycle. Escalation Protocols Unresolved issues stall execution in fast-moving environments. Structured escalation protocols define: What qualifies as a blocker requiring escalationTime thresholds for each escalation levelClear escalation chain (department → CDO → CEO)Documentation requirements for trackingResolution tracking and lesson captureThis prevents silent delays and ensures risk is surfaced early. Escalation becomes structured, not emotional. The Strategic Advantage of Controlled Growth When these governance components operate together, healthcare organizations gain: Clarity in authority – eliminating decision paralysisDiscipline in execution – structured rather than improvisedVisibility into risk – proactive rather than reactiveControlled technology expansion – integrated rather than fragmentedPredictable accountability – measured rather than assumedReduced compliance exposure – engineered rather than retrofittedGrowth becomes intentional rather than improvised. Compliance isn’t bolted on after an incident, it’s engineered into the organization’s architecture. This is the foundation upon which sustainable healthcare expansion is built. Not through limiting growth, but through designing the systems that make growth sustainable. Your Growth Architecture Assessment: Take Action Now The cost of waiting isn’t just inefficiency—it’s exponential risk compounding daily. Every new system, vendor relationship, and
Why Healthcare Startups Collapse From Rapid Growth

The hidden technical challenge that kills more healthcare companies than competition ever will The $10 Million Problem No One Talks About Picture this: Your healthcare startup is thriving. Patient appointments are booked solid. Revenue is climbing. Your team is energized. Then suddenly, everything starts falling apart. Your CRM crashes during peak hours. Compliance reports take weeks to generate. Staff spend more time fighting software than helping patients. Costs spiral while efficiency plummets. What started as a promising venture becomes an operational nightmare. This isn’t a story about bad luck or poor management. It’s about scalable infrastructure—a complex technical concept that determines whether your growth becomes sustainable success or expensive chaos. What Is Scalable Infrastructure? (The Building Blocks Explained) Think of scalable infrastructure like the foundation and framework of a skyscraper. You wouldn’t build a 50-story building on a foundation designed for a house. Similarly, you can’t grow a healthcare organization on systems designed for a small practice. Scalable infrastructure means building your operational foundation using modular architecture principles that can expand efficiently without breaking down. In simple terms, it’s the art of designing systems that grow stronger, not more fragile, as you add patients, locations, and staff. The core techniques include: But in healthcare, there’s an added layer of complexity: everything must remain compliant while scaling. The Healthcare Compliance Multiplier Effect Healthcare organizations face a unique challenge that makes infrastructure even more critical. Unlike a typical software company, you’re not just scaling technology—you’re scaling regulated technology. Every system must simultaneously comply with: When you scale from one location to five, you’re not just multiplying your infrastructure—you’re exponentially increasing your compliance surface area. A single oversight can trigger penalties, audits, or operational shutdowns. This is why government agencies like the Office of Inspector General provide extensive guidance resources including fraud alerts, advisory bulletins, and educational materials. They understand that compliance failures often stem from infrastructure problems, not intentional violations. Real-World Example: The Multi-Location Healthcare Practice Let’s walk through a practical example that illustrates these concepts in action. The Problem: A successful physical therapy practice wants to expand from 2 locations to 15. Their current setup includes: The Infrastructure Challenge: Simply copying their current approach would create: The Scalable Solution: Instead of replicating fragmented systems, they implement modular infrastructure: The result? Each new location launches with the same operational maturity as the established ones, compliance scales alongside growth, and costs remain predictable. The Three Pillars of Healthcare Infrastructure Scaling Pillar 1: Governance as Foundation Before deploying any technology, successful healthcare organizations establish governance frameworks that define: Think of governance as the architectural blueprint. You wouldn’t start construction without blueprints, yet many healthcare organizations deploy systems without clear governance structures. Pillar 2: Modular Operational Design Rather than accumulating software solutions, scalable organizations design integrated ecosystems where: This prevents “tool sprawl” the expensive accumulation of disconnected software subscriptions that create more problems than they solve. Pillar 3: Growth-Infrastructure Alignment The most critical aspect of healthcare scaling is synchronizing revenue growth with operational capacity. This means: Practical Applications: What This Looks Like in Practice Financial Discipline: Real-time burn-rate visibility, automated accounts receivable tracking, departmental cost transparency, and multi-location financial modeling that prevents SaaS subscription bloat from eroding margins. Human Capital Systems: Structured hiring workflows that scale consistently across locations, standardized performance review processes, OKR alignment frameworks, and compliance training that adapts to regulatory changes automatically. Technology Integration: CRM systems that share data securely across locations, client portals that maintain consistent user experience, communication platforms with proper access controls, and automation that reduces manual work without compromising compliance. Replication Frameworks: New location onboarding using proven templates, vendor relationship management that scales pricing advantages, standardized reporting that provides consistent visibility, and governance procedures that maintain quality standards regardless of size. The Cost of Getting It Wrong Healthcare organizations that scale without proper infrastructure face predictable problems: The financial impact is severe. Organizations often find themselves spending more on fixing infrastructure problems than they would have invested in building scalable systems from the beginning. Your Infrastructure Readiness Assessment Ask yourself these questions about your current operations: If you answered “no” to any of these questions, your infrastructure may not be ready for your growth ambitions. Conclusion: Building for Tomorrow’s Success Today Scalable infrastructure isn’t about buying more software or hiring more IT staff. It’s about architectural thinking, designing operational foundations that become stronger and more efficient as you grow, not more fragile and expensive. The healthcare organizations that thrive during expansion understand this fundamental truth: infrastructure isn’t a cost center, it’s a competitive advantage. When your systems scale efficiently, your team can focus on patient care instead of fighting operational chaos. The question isn’t whether you can afford to invest in scalable infrastructure. The question is whether you can afford not to. Ready to assess your infrastructure scalability? Start by mapping your current decision rights, system ownership, and data flows. The clarity you gain will either confirm you’re ready for growth or reveal the specific areas that need strengthening before you scale. Don’t Scale Your Problems, Scale Your Solutions Building scalable infrastructure isn’t something you have to figure out alone. At Business Navigators Consulting, we specialize in helping healthcare organizations design and implement the operational foundations they need to grow efficiently and compliantly. Whether you’re preparing for your first expansion or struggling with systems that can’t keep pace with your success, we can help you: Ready to build infrastructure that powers sustainable growth? Schedule a consultation to discuss your scaling challenges and discover how we can help you grow stronger, not just bigger. Schedule Your Infrastructure Assessment → Growth in healthcare requires more than ambition, it requires architecture. Build yours intentionally.